CT scan — facial sinuses · 12 January 2026TC dos seios da face · 12 de janeiro de 2026
Volumetric multi-detector CT, no IV contrast. Indication: facial trauma (post bicycle accident, 5 January 2026). Requesting physician: Dr. José Roberto Chodraui (CRM 54911). 707 axial slices — scrub the slider, scroll over the image, click-and-drag vertically, or use the arrow keys to navigate. Tomografia computadorizada multidetector volumétrica, sem contraste endovenoso. Indicação: trauma facial (após acidente de bicicleta, 5 de janeiro de 2026). Médico solicitante: Dr. José Roberto Chodraui (CRM 54911). 707 cortes axiais — arraste o controle, role o cursor sobre a imagem, clique e arraste verticalmente, ou use as setas do teclado para navegar.
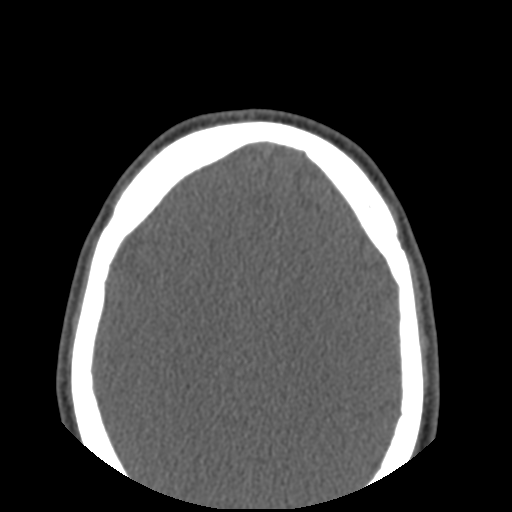
Radiologist's report (translated)
IdentifiersIdentificadores
- Patient. Joao Victor Creste Dias de Souza
- DOB. 17 October 1992
- Exam date. 12 January 2026
- Exam. Computed tomography of the facial sinuses
- Requesting physician. Dr. José Roberto Chodraui · CRM 54911
- Reference / Code. 4506971 / 0013393450323001
Indication & techniqueIndicação e técnica
- Clinical indication. Facial trauma.
- Technique. Volumetric acquisition of the facial sinuses on a multi-detector scanner, without venous contrast administration.
FindingsAchados
- Discrete bulging and soft-tissue irregularities in the right frontal region.
- Regional bone structures intact.
- Mucosal thickening of the left lateral wall of the sphenoid sinus, in the right maxillary sinus with obliteration of the ostiomeatal complex, and focal thickening of the floor of the left maxillary sinus. Normal transparency of the remaining facial sinuses. Left ostiomeatal complex unobstructed. Presence of an accessory ostium in the medial wall of the right maxillary sinus.
- Asymmetric inferior nasal turbinates — smaller on the right side.